In this upcoming episode, Dr. Meier will discuss how people move differently in the presence of (or in anticipation of) pain. Changes in motor control may play an important role in musculoskeletal pain. His lab uses a cross-disciplinary approach that combines neuroscience and movement biomechanics to provide new insights into the role of potential interactions between movement behavior, psychological factors and supraspinal mechanisms in the development and maintenance of persistent low back pain. We’ll touch also on fear avoidance and pain related movement avoidance. Dr. Michael L. Meier is a senior pain researcher and group leader at the Department of Chiropractic Medicine at the University of Zurich. He received his master’s degree in neuropsychology and his doctorate in cognitive neuroscience from the University of Zurich, focusing on the processing of pain and nociception in the brain. In 2019, he received a grant from the Swiss National Science Foundation (SNF) to study the role of movement behavior and cortical processes in the development and persistence of low back pain. A hallmark of his work is linking research from different disciplines such as biomechanics, neuroscience, and psychology, shedding light on novel interacting pathomechanisms underlying persistent low back pain whose pathoanatomical cause is often unclear.
Posts

Dr. Haussler graduated from The Ohio State University, College of Veterinary Medicine in 1988 and completed a small animal internship in Sacramento, CA. To further his training in the conservative management of spinal-related disorders, he pursued human training at Palmer College of Chiropractic-West and completed a veterinary chiropractic certification program in 1993. He attended the University of California-Davis to attain a PhD focusing on spinal pathology and pelvic biomechanics in Thoroughbred racehorses. Currently, he is an Associate Professor at the Orthopaedic Research Center at Colorado State University and is involved in teaching, clinical duties, and research into the objective assessment of musculoskeletal pain, spinal dysfunction and the application of physical therapy and rehabilitation. Please comment below if you have any questions for us during the interview. I might choose some of them for our conversation.
 Subacute and chronic patients with MRI confirmed symptomatic disc herniation treated with spinal manipulation were statistically (and clinically) significantly more likely to report improvement at 3 months compared with the nerve root injection. This prospective cohort study had 104 patients, 52 patients treated with cervical nerve root injection (CNRI) and 52 patients treated with spinal manipulation by a chiropractor. Baseline numerical rating scale (NRS) pain data were collected. Three months after treatment, numerical rating score pain levels were recorded and overall “improvement” was assessed using the Patient Global Impression of Change scale. Responses that were “much better” or “better” were considered to be “improved.” The proportion of patients “improved” was calculated for each treatment method and compared. The NRS and NRS change scores for the 2 groups were compared at baseline and 3 months. Results showed that there was no significant difference in outcomes between acute patients treated with cervical nerve root blocks and those treated with spinal manipulation at 3 months. However, when comparing the 3-month outcomes for the subacute/chronic patients, more than 78% of patients treated with SMT reported clinically relevant improvement compared with 37.5% of patients receiving a single CNRI. There were no adverse events for patients in either treatment group and the cost of treatment was similar for the 2 treatment procedures.
Subacute and chronic patients with MRI confirmed symptomatic disc herniation treated with spinal manipulation were statistically (and clinically) significantly more likely to report improvement at 3 months compared with the nerve root injection. This prospective cohort study had 104 patients, 52 patients treated with cervical nerve root injection (CNRI) and 52 patients treated with spinal manipulation by a chiropractor. Baseline numerical rating scale (NRS) pain data were collected. Three months after treatment, numerical rating score pain levels were recorded and overall “improvement” was assessed using the Patient Global Impression of Change scale. Responses that were “much better” or “better” were considered to be “improved.” The proportion of patients “improved” was calculated for each treatment method and compared. The NRS and NRS change scores for the 2 groups were compared at baseline and 3 months. Results showed that there was no significant difference in outcomes between acute patients treated with cervical nerve root blocks and those treated with spinal manipulation at 3 months. However, when comparing the 3-month outcomes for the subacute/chronic patients, more than 78% of patients treated with SMT reported clinically relevant improvement compared with 37.5% of patients receiving a single CNRI. There were no adverse events for patients in either treatment group and the cost of treatment was similar for the 2 treatment procedures.
Reference: Peterson CK, Pfirrmann CW, Hodler J, Leemann S, Schmid C, Anklin B, Humphreys
BK. Symptomatic, Magnetic Resonance Imaging-Confirmed Cervical Disk Herniation Patients: A Comparative-Effectiveness Prospective Observational Study of 2 Age- and Sex-Matched Cohorts Treated With Either Imaging-Guided Indirect Cervical Nerve Root Injections or Spinal Manipulative Therapy. J Manipulative Physiol Ther. 2016 Mar-Apr;39(3):210-7.
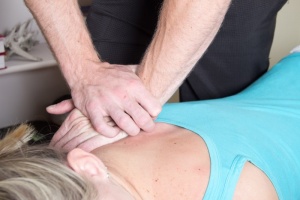 Spinal manipulation (SM) can improve function and reduce spinal disability. SM also provides pain relief for many disorders such as back pain and neck pain. Pain induces changes in both the central and peripheral nervous systems. The mechanisms by which SM alters musculoskeletal pain are still not completely known. Current evidence however suggests that SM is associated with neurophysiological responses including rapid hypoalgesia with simultaneous sympathetic and motor system excitation. Animal studies have shown that analgesia provided by joint mobilization involves serotonin and noradrenaline receptors in the spinal cord.
Spinal manipulation (SM) can improve function and reduce spinal disability. SM also provides pain relief for many disorders such as back pain and neck pain. Pain induces changes in both the central and peripheral nervous systems. The mechanisms by which SM alters musculoskeletal pain are still not completely known. Current evidence however suggests that SM is associated with neurophysiological responses including rapid hypoalgesia with simultaneous sympathetic and motor system excitation. Animal studies have shown that analgesia provided by joint mobilization involves serotonin and noradrenaline receptors in the spinal cord.
A new investigation sought to determine the response of several other biochemical markers of pain and stress to SM. Specifically, three neuropeptides (neurotensin, oxytocin, orexin A) and a glucorticoid hormone (cortisol) were studied. The authors note that the neuropeptides have been associated with hypoalgesia and pain modulation and that cortisol plays an analgesic role in the stress response. Recent theories have suggested that chronic pain could be partially maintained in a facilitated state due to maladaptive responses in the presence of recurrent stressful situations. To date there is a lack of studies analyzing these specific biomarkers in relation to SM.
The purpose of this study was to determine the effect of cervical or thoracic manipulation on neurotensin (NT), oxytocin, orexin A, and cortisol levels. Experimenters examined both spinal regions because they thought there may be a difference in anti-nociceptive effect between the cervical spine and thoracic spine.
Participants included graduate students from Spain. All subjects were asymptomatic and were excluded if there was a contraindication to manipulation, history of whiplash or surgery, pain in the last month, SM in the last 2 months. Thirty asymptomatic subjects were randomly divided into 3 groups: cervical manipulation (n = 10), thoracic manipulation (n = 10), and non-manipulation (control) (n = 10). Although it is not explicitly stated in the article, I presume the manipulations were performed by physical therapists since the lead authors were PT’s. Manipulations consisted of supine ‘anterior’ thoracic spine manipulations, and rotary type cervical manipulations. Blood samples were extracted before, immediately after, and 2 hours after each intervention by way of venipuncture of the cephalic vein. Neurotensin, oxytocin, and orexin A were determined in plasma using enzyme-linked immuno assay. Cortisol was measured by microparticulate enzyme immuno assay in serum samples.
Results
Neurotensin (NT)
- Statistically significant increases in neurotensin occurred in both the thoracic and cervical manipulation groups compared to controls post-intervention with the greatest increase occurring immediately following manipulation
- Cervical spine manipulation produced a slightly larger increase in neurotensin
Orexin A
- No statistically significant changes were noted in orexin A levels following treatment
Oxytocin
- Statistically significant increases in oxytocin occurred in both the thoracic and cervical manipulation groups compared to controls post-intervention with the greatest increase occurring immediately following manipulation
- Cervical spine manipulation produced a significantly larger increase in oxytocin compared to thoracic manipulation
Cortisol
- A significant increase in cortisol occurred in the cervical manipulation group compared to controls and the thoracic manipulation group immediately post-intervention
- However, a significant decrease in cortisol was found at 2 hrs post intervention in the thoracic SM group compared with pre-intervention values
- A non-significant decrease in cortisol was found also found at 2 hrs post intervention in the cervical SM group compared with pre-intervention values
Discussion
NT is an endogenous peptide with broad spectrum of central and peripheral activities, including modulation of pain signal transmission and perception. NT behaves as a neurotransmitter in the brain and as a hormone in the gut. Because of its association with a wide variety of neurotransmitters, NT has been implicated in the pathophysiology of several CNS disorders such as schizophrenia, drug abuse, Parkinson’s disease (PD), pain, central control of blood pressure, eating disorders, as well as, cancer and inflammation. Note that the antinociceptive effects of NT are independent from opioid antinociception.
Increased oxytocin following SM could be partly responsible for the analgesic effect linked to manual therapy techniques due to the activation of descending pain-inhibitory pathways.
Cortisol is a potent anti-inflammatory that functions to mobilize glucose reserves for energy and modulate inflammation. Ultimately, a prolonged or exaggerated stress response may perpetuate cortisol dysfunction, widespread inflammation, and pain. SM in this study led to an immediate increase in cortisol followed by a significant 2 hour decrease in levels with thoracic manipulation and a decrease in 2 hr levels with cervical manipulation.
Key Points
- SM can modify several biochemical markers of pain and stress
- These findings suggest that descending inhibitory pathway mechanisms may be involved in the physiological effects that follow SM
- The effect size for the cervical manipulation group was larger than that for the thoracic manipulation group suggesting an increase in the activation of the possible descending inhibitory pathway mechanisms after cervical manipulation compared to thoracic manipulation
 The application of spinal manipulative therapy (SMT) is a cost-effective and widely recognized manual intervention used by a variety of health care professionals in the management of musculoskeletal pain. A growing body of scientific evidence supports the use of SMT for the treatment of a broad range of musculoskeletal disorders citing short-term antinociceptive (pain-relieving) effects and restoration of normal joint mechanics.
The application of spinal manipulative therapy (SMT) is a cost-effective and widely recognized manual intervention used by a variety of health care professionals in the management of musculoskeletal pain. A growing body of scientific evidence supports the use of SMT for the treatment of a broad range of musculoskeletal disorders citing short-term antinociceptive (pain-relieving) effects and restoration of normal joint mechanics.
Last year, about this time, I wrote about a systematic review that found spinal manipulation therapy (SMT) has a pain reducing effect as measured by pressure pain thresholds (PPT). Additionally, the effect of SMT on pain reduction was statistically significant at remote locations (for example, adjusting the neck yielded reduction in pain at the elbow).
A new study has emerged in the scientific literature that advances our understanding of the topic (Srbely et al, 2013). The authors note that although the pathophysiology of myofascial pain syndrome (MPS) is still unclear, research suggests that myofascial trigger points (MTPs) play an fundamental role in the generation and clinical manifestation of MPS. However, it is currently unknown if the antinociceptive effects of SMT in myofascial tissues are manifest predominantly via regional or general mechanisms, or a combination of both. A study was needed to specifically investigate the hypothesis that SMT evokes robust antinociceptive effects in MTPs preferentially located within neurosegmentally linked myofascial tissues.
Srbely et al conducted the study through the University of Guelph. The study was a single session, single blinded, randomized controlled intervention. The primary inclusion criterion was the presence of a clinically identifiable MTP locus (active or latent) within the right infraspinatus and right gluteus medius muscles. The primary diagnostic criterion used to clinically identify the trigger point locus was ‘a palpable hyperirritable nodule nested within a taut band of skeletal muscle; sustained ischemic pressure over the trigger point locus elicited a dull achy regional pain or discomfort.’ Exclusion criteria encompassed conditions that would affect normal somatosensory processing.
Thirty-six participants qualified for the study and were randomly assigned to test or control groups. Two chiropractors saw participants at an urban outpatient clinic. One chiropractor performed the history, exam and manipulations while the other chiropractor (blinded to treatment allocation) detected the trigger points and measured all PPTs. The primary outcome was PPT values from infraspinatus and gluteus medius muscles. The infraspinatus was chosen due to its innervation from the manipulated segment (C5-6). The gluteus medius acted as a regional control point (L4-S1 innervation).
PPT was measured with a force gauge (Newtons) over the trigger point locus (infraspinatus, gluteus medius) and was defined as the force necessary to elicit the onset of a deep dull achy local discomfort and/or referred pain. Measurements were taken at 1,5, 10, and 15 minutes postintervention. In order to specifically compare regional antinociceptive effects between intervention groups, the authors also calculated the PPT difference (PPTdiff) between infraspinatus and gluteus medius trigger points at each time interval within each participant. Participants received a rotary type manipulation to the C5-6 segment in a supine posture. Additionally, a drop piece mechanism was used to aid in the high velocity low amplitude thrust. Control participants received a sham manipulation. The sham consisted of rotating the neck of the participant, supporting the neck of the participant with the clinician’s forearm under the headpiece and a thrust of the forearm into the headpiece. It is noted that the contact hand did not thrust and did not create ‘a real manipulation’ of any segment.
Results:
- there was a significantly increased PPT threshold for infraspinatus trigger points in treated participants compared to controls at all time intervals beyond baseline
- there was a significantly increased PPT threshold for infraspinatus compared to gluteus medius before and after manipulation at all time intervals beyond baseline
- no significant differences in PPT scores were observed at any time interval when comparing test gluteus medius, control infraspinatus, and control gluteus medius groups
- there were significant increases in PPTdiff in the test group vs controls at all time intervals beyond baseline
Key Findings:
- This study suggests that SMT evokes statistically significant short-term increases in PPT in segmentally related myofascial tissues in young adults
- Decreased pressure sensitivity (increased PPT score) was observed at all time intervals beyond baseline within neurologically linked infraspinatus muscle after real, but not sham, manipulation
- The peak antinociceptive effect was measured as a 36% decrease in pressure sensitivity from baseline values and was recorded at 5 minutes postSMT
So, what does this study tell us? It suggests that SMT evokes robust regional antinociceptive effects in myofascial tissues. It also provides important evidence to support further research into the potential benefit and role of SMT in the management of chronic widespread pain syndromes including myofascial pain, and fibromyalgia.
Episode

Drs. Jim Whedon and Brian Anderson join me for a discussion about their R15 award involving 3 Medicare neck pain cohort studies.
Jim Whedon DC, MS is a Senior Health Services Researcher at Southern California University of Health Sciences and Adjunct Professor at The Dartmouth Institute for Health Policy and Clinical Practice. He has authored more than 65 peer reviewed publications. Dr. Whedon’s research focuses on evaluation of the quality and accessibility of non-pharmacological therapies for spine pain. He is a recipient of the Jerome F. McAndrews DC Memorial Research Fund Award from NCMIC Foundation and the Scott Haldeman Award for Outstanding Research from the World Federation of Chiropractic.
Dr. Anderson is a health services researcher and 2004 graduate of National University of Health Sciences. He has 20 years of experience across clinical practice, teaching, and research. His efforts have been focused on research full-time since completing his PhD in 2019. He served as a faculty member at the Palmer Center for Chiropractic Research for five years before transitioning to the University of Pittsburgh. His research examines healthcare utilization and outcomes in spinal pain disorders using administrative claims, electronic health records, and survey data. Additional research interests include research-capacity building in chiropractic and other CIH institutions as well as evidence synthesis. At the University of Pittsburgh, he engages in interdisciplinary research initiatives, advises faculty and trainees, and contributes to the integration of research methodologies into the academic curriculum.
Here is the video for this episode:
Here are Dr. Whedon’s researchgate profile as well as Dr. Anderson’s researchgate profile.
The articles that are discussed in this episode are found below:
|
1.
|
Observational Study of the Safety of Chiropractic vs Medical Care Among Older Adults With Neck Pain.
Whedon JM, Anderson B, Mackenzie TA, Grout L, Moonaz S, Lurie JD, Haldeman S.
J Manipulative Physiol Ther. 2025 Sep 9:S0161-4754(25)00002-8. doi: 10.1016/j.jmpt.2025.07.002. Online ahead of print.
PMID: 40923947 |
|
2.
|
Comparative Cost Analysis of Neck Pain Treatments for Medicare Beneficiaries.
Anderson BR, MacKenzie TA, Grout LM, Whedon JM.
Arch Phys Med Rehabil. 2025 May;106(5):801-804. doi: 10.1016/j.apmr.2025.01.467. Epub 2025 Feb 14.
PMID: 39955668 |
|
3.
|
Patterns of initial treatment and subsequent care escalation among medicare beneficiaries with neck pain: a retrospective cohort study.
Anderson BR, MacKenzie TA, Lurie JD, Grout L, Whedon JM.
Eur Spine J. 2025 Feb;34(2):724-730. doi: 10.1007/s00586-024-08581-3. Epub 2024 Dec 26.
PMID: 39722095 |

Dr. Felipe C. K. Duarte graduated from Feevale University-Brazil in 2008. He has clinical experience as a chiropractor and three other degrees (postgrad dip: Exercise Physiology; MSc: Human Physiology; PhD: Neuroscience). Between 2019 and 2023, he held a research-intensive position at CMCC-Toronto as a postdoctoral fellow and research associate in a rehab research-focused hospital (KITE-Toronto Rehab Institute-UHN, Toronto). Since 2023 Felipe is a senior lecturer at the School of Health, Medical and Applied Sciences, Chiropractic Discipline, Central Queensland University, Australia. He also holds Adjunct professor status at the Canadian Memorial Chiropractic College.
His research interests aim to (1) investigate the neurobiological and neuromechanical mechanisms underlying highly prevalent disabling chronic musculoskeletal conditions, such as chronic spinal pain, neuropathic pain, fibromyalgia, myofascial pain syndrome, and osteoarthritis, which are of great concern to public health systems; (2) Investigate the underlying mechanisms of rehab strategies such as force-based mechanotherapy (e.g., spinal manipulation), focusing on the neurobiological and neuro-immune factors; (3) use these biological determinants to explore their potential for patient stratification in chronic MSK conditions and to spinal manipulation (e.g., responders x non-responders).
Felipe has experience in various methodologies and study designs to address his research interests, which range from molecular biology to neuroimaging and clinical epidemiology. Felipe also possesses direct teaching experience in Biochemistry, Physiology, Neuromusculoskeletal Anatomy, Neuroanatomy, and Clinical Neurological Assessment and Diagnosis at both undergraduate and postgraduate levels.
Visit Dr. Duarte’s research at researchgate.net and view his faculty page.
Here are the articles we discuss during this episode:
|
1.
|
Myofascial Pain as an Unseen Comorbidity in Osteoarthritis: A Scoping Review.
Duarte FCK, Chien R, Ghazinour G, Murnaghan K, West DWD, Kumbhare DA.
Clin J Pain. 2023 Apr 1;39(4):188-201. doi: 10.1097/AJP.0000000000001102.
PMID: 36943163 Review. |
|
2.
|
Effects of Distinct Force Magnitude of Spinal Manipulative Therapy on Blood Biomarkers of Inflammation: A Proof of Principle Study in Healthy Young Adults.
Duarte FCK, Funabashi M, Starmer D, Partata WA, West DWD, Kumbhare DA, Injeyan S.
J Manipulative Physiol Ther. 2022 Jan;45(1):20-32. doi: 10.1016/j.jmpt.2022.03.012. Epub 2022 Jun 25.
PMID: 35760595 Clinical Trial. |
|
3.
|
Re-Examining Myofascial Pain Syndrome: Toward Biomarker Development and Mechanism-Based Diagnostic Criteria.
Duarte FCK, West DWD, Linde LD, Hassan S, Kumbhare DA.
Curr Rheumatol Rep. 2021 Jul 8;23(8):69. doi: 10.1007/s11926-021-01024-8.
PMID: 34236529 Review. |
|
4.
|
Spinal Manipulation Therapy Improves Tactile Allodynia and Peripheral Nerve Functionality and Modulates Blood Oxidative Stress Markers in Rats Exposed to Knee-Joint Immobilization.
Duarte FCK, Kolberg C, Riffel APK, Souza JA, Belló-Klein A, Partata WA.
J Manipulative Physiol Ther. 2019 Jul;42(6):385-398. doi: 10.1016/j.jmpt.2018.11.023. Epub 2019 Jul 30.
PMID: 31371096 |
|
5.
|
Spine-Adjusting Instrument (Impulse®) Attenuates Nociception and Modulates Oxidative Stress Markers in the Spinal Cord and Sciatic Nerve of a Rat Model of Neuropathic Pain.
da Silva FBO, Santos MDCQ, da Silva TCB, Facchini D, Kolberg A, Barros RR, Silveira EMS, Kroth A, Duarte FCK, Vassoler JM, Kolberg C, Partata WA.
Pain Med. 2022 Apr 8;23(4):761-773. doi: 10.1093/pm/pnab167.
PMID: 33993301 |
Here is a link to Clinical Compass. While there, check out the Evidence Center, Clinical Guidelines, and various other resources!

In this interview, Dr. Scali discusses with me the upper cervical spine and myodural bridge (connective tissue between suboccipital muscles and the cervical spinal dura mater). Dr. Frank Scali grew up in Valley Stream, Long Island, New York, and studied Neuroscience at Stony Brook University. In 2009, he received his Doctorate in Chiropractic at Logan University in Chesterfield, Missouri. During his time in medical school, Dr. Frank Scali professionally prosected cadaveric specimens for Gray’s Anatomy and illustrated for multiple journals and textbooks, including the Oxford Handbook of Bariatric Surgery. While attending medical school, he published multiple non-variant anatomical findings in the medical literature and served as an Ad Hoc Reviewer in Journals such as The Spine Journal, The Anatomical Record, Surgical and Radiological Anatomy, and others. In 2018, he graduated with his MD from AUC School of Medicine with fifty-four publications, including textbook contributions and a patent for a medical device.
Dr. Scali is board certified in Chiropractic and Medicine. His current title is Assistant Professor of Medical Education and Anatomy at the California University of Science and Medicine. At CUSM, Dr. Scali serves as the Director of the ATLAS Lab Center, is the Director of the USMLE Board Preparation, and is the Course Director for MSK/Derm, Surgical Anatomy, and the Step 1/2CK Board Prep course. He was inducted into the Sigma Xi Scientific Research & Honor Society in 2020 and serves on the Editorial Board for the Journal of Medicine since 2019. As Assistant Professor of Medical Education, Dr. Scali has achieved dozens of teaching awards in Medical Foundations, MSK/Derm, Neuroscience, Reproductive Medicine, and Medical Board Preparation courses. Because of his innovative teaching style, in 2021, Dr. Scali became the inaugural recipient of the Robert Suskind & Leslie Lewinter-Suskind Pre-Clinical Faculty of the Year award.
Visit Dr. Scali’s research at researchgate.net and view his faculty page.
Here are the articles we discuss during this episode:
| 1. | Anatomical connection between the rectus capitis posterior major and the dura mater.Scali F, Marsili ES, Pontell ME.Spine (Phila Pa 1976). 2011 Dec 1;36(25):E1612-4. doi: 10.1097/BRS.0b013e31821129df.PMID: 21278628 |
| 2. | Investigation of meningomyovertebral structures within the upper cervical epidural space: a sheet plastination study with clinical implications.Scali F, Pontell ME, Nash LG, Enix DE.Spine J. 2015 Nov 1;15(11):2417-24. doi: 10.1016/j.spinee.2015.07.438. Epub 2015 Jul 22.PMID: 26210227 |
| 3. | Histological analysis of the rectus capitis posterior major’s myodural bridge.Scali F, Pontell ME, Enix DE, Marshall E.Spine J. 2013 May;13(5):558-63. doi: 10.1016/j.spinee.2013.01.015. Epub 2013 Feb 11.PMID: 23406969 |
| 4. | The Posterior Atlantooccipital Membrane: The Anchor for the Myodural Bridge and Meningovertebral Structures.Scali F, Ohno A, Enix D, Hassan S.Cureus. 2022 May 30;14(5):e25484. doi: 10.7759/cureus.25484. eCollection 2022 May.PMID: 35686279 Free PMC article. |

Dr. Carlos Gevers joins me to discuss mechanisms of spinal manipulation, particularly as they relate to central sensitization and neuroinflammation. He also shares a study on Tumor Necrosis Factor-Alpha in Urine Samples of Patients With Chronic Low Back Pain Undergoing Chiropractic Care.
Carlos Gevers Montoro is a second-generation chiropractor. He graduated from Life Chiropractic College West in 2003 as Valedictorian and the recipient of the Clinical Excellence Citation award. After practicing for a few years in Spain and France, he was instrumental in the opening of the Madrid College of Chiropractic (MCC), where he still lectures. His contributions at the MCC were mostly related to the clinical sciences. In parallel, he served for seven years as the President of the Spanish Chiropractic Association, being involved in chiropractic politics and policy at the national and international level.
In 2018 he decided to switch gears and take a completely new path in the research arena. He started his PhD in Pain Neurosciences at UQTR – University of Montreal joint program under the supervision of Prof. Mathieu Piché. His PhD studies are partially funded, by a prestigious grant from the Government of Quebec. His line of research and his first publications are mostly focused on mechanisms of spinal manipulation, particularly as they relate to central sensitization and neuroinflammation. These two phenomena seem to be strongly implicated in the development of chronic pain syndrome and other conditions.
Check out Dr. Carlos Gevers researchgate profile page.
Here are the articles we discuss in this episode:
| 1. | Presence of Tumor Necrosis Factor-Alpha in Urine Samples of Patients With Chronic Low Back Pain Undergoing Chiropractic Care: Preliminary Findings From a Prospective Cohort Study.Gevers-Montoro C, Romero-Santiago M, Losapio L, Conesa-Buendía FM, Newell D, Álvarez-Galovich L, Piché M, Ortega-De Mues A.Front Integr Neurosci. 2022 Apr 12;16:879083. doi: 10.3389/fnint.2022.879083. eCollection 2022.PMID: 35492573 Free PMC article. |
| 2. | Chiropractic Spinal Manipulation Prevents Secondary Hyperalgesia Induced by Topical Capsaicin in Healthy Individuals.Gevers-Montoro C, Provencher B, Northon S, Stedile-Lovatel JP, Ortega de Mues A, Piché M.Front Pain Res (Lausanne). 2021 Jul 20;2:702429. doi: 10.3389/fpain.2021.702429. eCollection 2021.PMID: 35295504 Free PMC article. |
| 3. | Neurophysiological mechanisms of chiropractic spinal manipulation for spine pain.Gevers-Montoro C, Provencher B, Descarreaux M, Ortega de Mues A, Piché M.Eur J Pain. 2021 Aug;25(7):1429-1448. doi: 10.1002/ejp.1773. Epub 2021 Apr 15.PMID: 33786932 Review. |

Dr. Ken Weber and I discuss his research pursuits which involve: 1) developing imaging modalities that are more sensitive and specific to the pathology, providing more diagnostic, prognostic, and predictive information; 2) providing more quantitative information to the clinician; and 3) using these measures to better understand the nervous system and how it functions, the neurophysiology of pain, how treatments work, and why certain treatments work for some patients but not for others. Dr. Ken Weber is an Instructor in the Department of Anesthesia, Perioperative and Pain Medicine at Stanford University. He obtained his Doctor of Chiropractic from Palmer College of Chiropractic Florida in 2009 and then completed a PhD in neuroscience at Northwestern University in 2016, specializing in movement and rehabilitation science. Ken’s research intersects clinical pain research and advanced MRI techniques with an emphasis on brain, spinal cord, and musculoskeletal imaging. His research aims to better understand the neural and musculoskeletal changes underlying clinical pain conditions, the mechanisms of treatments, and predictors for recovery. Ken is currently supported by a K23 Mentored Patient-Oriented Research Career Development Award from the National Institute of Neurological Disorders and Stroke of the National Institutes of Health. His previous funding has included the National Center for Complementary and Integrative Health, the National Institute on Drug Abuse, and the NCMIC Foundation, Inc.
I’d also like to point out that Ken was recently selected to be part of the CARL (Chiropractic Academy for Research Leadership) program.
View Dr. Weber‘s research at researchgate.net.
Here are some of the papers we discuss in this episode.
| 1. | Machine Learning for the Prediction of Cervical Spondylotic Myelopathy: A Post Hoc Pilot Study of 28 Participants. |
| Hopkins BS, Weber KA 2nd, Kesavabhotla K, Paliwal M, Cantrell DR, Smith ZA. | |
| World Neurosurg. 2019 Jul;127:e436-e442. doi: 10.1016/j.wneu.2019.03.165. Epub 2019 Mar 25. | |
| PMID: 30922901 [PubMed – indexed for MEDLINE] | |
| Similar articles |
| 2. | Are Magnetic Resonance Imaging Technologies Crucial to Our Understanding of Spinal Conditions? |
| Crawford RJ, Fortin M, Weber KA 2nd, Smith A, Elliott JM. | |
| J Orthop Sports Phys Ther. 2019 May;49(5):320-329. doi: 10.2519/jospt.2019.8793. Epub 2019 Mar 26. | |
| PMID: 30913967 [PubMed – in process] | |
| Similar articles |
| 3. | Lateral Corticospinal Tract Damage Correlates With Motor Output in Incomplete Spinal Cord Injury. |
| Smith AC, Weber KA 2nd, O’Dell DR, Parrish TB, Wasielewski M, Elliott JM. | |
| Arch Phys Med Rehabil. 2018 Apr;99(4):660-666. doi: 10.1016/j.apmr.2017.10.002. Epub 2017 Oct 26. | |
| PMID: 29107041 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
| 4. | Evidence for decreased Neurologic Pain Signature activation following thoracic spinal manipulation in healthy volunteers and participants with neck pain. |
| Weber Ii KA, Wager TD, Mackey S, Elliott JM, Liu WC, Sparks CL. | |
| Neuroimage Clin. 2019;24:102042. doi: 10.1016/j.nicl.2019.102042. Epub 2019 Oct 18. | |
| PMID: 31670070 [PubMed – in process] Free PMC Article | |
| Similar articles |
| 5. | Deep Learning Convolutional Neural Networks for the Automatic Quantification of Muscle Fat Infiltration Following Whiplash Injury. |
| Weber KA, Smith AC, Wasielewski M, Eghtesad K, Upadhyayula PA, Wintermark M, Hastie TJ, Parrish TB, Mackey S, Elliott JM. | |
| Sci Rep. 2019 May 28;9(1):7973. doi: 10.1038/s41598-019-44416-8. | |
| PMID: 31138878 [PubMed – in process] Free PMC Article | |
| Similar articles |

Tue Secher Jensen graduated from the University of Southern Denmark in 2002 and has been working as a researcher since his student years. After graduation, he worked as a chiropractic intern and as a chiropractor for a couple of years alongside his work as a research assistant. In 2009, he defended his PhD thesis on the prevalence, development and clinical value of Modic changes in the general population. From 2013 to 2016, he was employed as a senior researcher and clinical associate professor at the Spine Centre of Southern Denmark and since 2013 he has also been employed as a senior researcher at the Nordic Institute of Chiropractic and Clinical Biomechanics (NIKKB). Since 2017, Tue Secher Jensen has been employed at the Diagnostic Centre – Imaging Sector at the Regional Hospital in Silkeborg, Denmark, as a chiropractor doing research and reading spinal MRI. From 2018 to 2019 he was an associate professor at the Department of Clinical Medicine at Aarhus University. Tue Secher Jensen was recently (January 1st 2020) appointed, along with Lise Hestbaek (who has previously been on the podcast), as professors at the Department of Sports Science and Clinical Biomechanics at SDU.
Tue’s research has primarily focused on the clinical value of MRI findings in people with back pain. In recent years his research focus has shifted more towards clinical guidelines, knowledge translation and implementation.
See more of Tue’s research at researchgate.net.
The articles we discuss in this episode include:
| 1. | Systematic literature review of imaging features of spinal degeneration in asymptomatic populations. |
| Brinjikji W, Luetmer PH, Comstock B, Bresnahan BW, Chen LE, Deyo RA, Halabi S, Turner JA, Avins AL, James K, Wald JT, Kallmes DF, Jarvik JG. | |
| AJNR Am J Neuroradiol. 2015 Apr;36(4):811-6. doi: 10.3174/ajnr.A4173. Epub 2014 Nov 27. Review. | |
| PMID: 25430861 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
| 2. | MRI Findings of Disc Degeneration are More Prevalent in Adults with Low Back Pain than in Asymptomatic Controls: A Systematic Review and Meta-Analysis. |
| Brinjikji W, Diehn FE, Jarvik JG, Carr CM, Kallmes DF, Murad MH, Luetmer PH. | |
| AJNR Am J Neuroradiol. 2015 Dec;36(12):2394-9. doi: 10.3174/ajnr.A4498. Epub 2015 Sep 10. Review. | |
| PMID: 26359154 [PubMed – indexed for MEDLINE] Free Article | |
| Similar articles |
| 3. | Magnetic resonance imaging findings as predictors of clinical outcome in patients with sciatica receiving active conservative treatment. |
| Jensen TS, Albert HB, Sorensen JS, Manniche C, Leboeuf-Yde C. | |
| J Manipulative Physiol Ther. 2007 Feb;30(2):98-108. | |
| PMID: 17320730 [PubMed – indexed for MEDLINE] | |
| Similar articles |
| 4. | Natural course of disc morphology in patients with sciatica: an MRI study using a standardized qualitative classification system. |
| Jensen TS, Albert HB, Soerensen JS, Manniche C, Leboeuf-Yde C. | |
| Spine (Phila Pa 1976). 2006 Jun 15;31(14):1605-12; discussion 1613. | |
| PMID: 16778696 [PubMed – indexed for MEDLINE] | |
| Similar articles |
| 5. | Modic changes, possible causes and relation to low back pain. |
| Albert HB, Kjaer P, Jensen TS, Sorensen JS, Bendix T, Manniche C. | |
| Med Hypotheses. 2008;70(2):361-8. Epub 2007 Jul 10. | |
| PMID: 17624684 [PubMed – indexed for MEDLINE] | |
| Similar articles |
| 6. | Vertebral endplate signal changes (Modic change): a systematic literature review of prevalence and association with non-specific low back pain. |
| Jensen TS, Karppinen J, Sorensen JS, Niinimäki J, Leboeuf-Yde C. | |
| Eur Spine J. 2008 Nov;17(11):1407-22. doi: 10.1007/s00586-008-0770-2. Epub 2008 Sep 12. Review. | |
| PMID: 18787845 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
| 7. | Modic changes-Their associations with low back pain and activity limitation: A systematic literature review and meta-analysis. |
| Herlin C, Kjaer P, Espeland A, Skouen JS, Leboeuf-Yde C, Karppinen J, Niinimäki J, Sørensen JS, Storheim K, Jensen TS. | |
| PLoS One. 2018 Aug 1;13(8):e0200677. doi: 10.1371/journal.pone.0200677. eCollection 2018. | |
| PMID: 30067777 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
| 8. | Antibiotic treatment in patients with chronic low back pain and vertebral bone edema (Modic type 1 changes): a double-blind randomized clinical controlled trial of efficacy. |
| Albert HB, Sorensen JS, Christensen BS, Manniche C. | |
| Eur Spine J. 2013 Apr;22(4):697-707. doi: 10.1007/s00586-013-2675-y. Epub 2013 Feb 13. | |
| PMID: 23404353 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
 Dr. de Luca and I discuss her research on spinal pain in the elderly and chiropractic. Katie de Luca is a post-doctoral research fellow in the Department of Chiropractic at Macquarie University. She is a chiropractor in clinical practice, however her research focuses on the epidemiology and management of musculoskeletal conditions, with expertise in the elderly. In 2016 she was awarded her PhD from the University of Newcastle, School of Medicine and Public Health. Her thesis explored the experience of pain in women with arthritis, and resulted in substantial contributions to the fields of rheumatology, pain and ageing research. She has 25 peer-reviewed journal publications and more than 50 conference presentations, which includes several invited keynote presentations on back pain in the elderly. These have been at regional, national and international conferences in gerontology, pain, public health and chiropractic forums. She is on the editorial boards of Chiropractic and Manual Therapies and JMPT, and peer-reviews for another 13 journals. She has received several large competitive grants, most recently being awarded in excess of $400,00 in an industry led grant from the Australia Chiropractors Association to perform a longitudinal study on back pain in older Australians who present to a chiropractor for treatment of their low back pain. She has won many research prizes, including 1st prize at the World Federation of Chiropractic Biennial Conference in Washington DC (March, 2017). She is actively on the board for the Chiropractic Australia Research Foundation, and is the Research Chair for Sports Chiropractic Australia. She is one of only 13 CARL Fellows, a group which she is privileged to be a part of. She hopes to be a leading chiropractic researcher on spinal pain in the elderly.
Dr. de Luca and I discuss her research on spinal pain in the elderly and chiropractic. Katie de Luca is a post-doctoral research fellow in the Department of Chiropractic at Macquarie University. She is a chiropractor in clinical practice, however her research focuses on the epidemiology and management of musculoskeletal conditions, with expertise in the elderly. In 2016 she was awarded her PhD from the University of Newcastle, School of Medicine and Public Health. Her thesis explored the experience of pain in women with arthritis, and resulted in substantial contributions to the fields of rheumatology, pain and ageing research. She has 25 peer-reviewed journal publications and more than 50 conference presentations, which includes several invited keynote presentations on back pain in the elderly. These have been at regional, national and international conferences in gerontology, pain, public health and chiropractic forums. She is on the editorial boards of Chiropractic and Manual Therapies and JMPT, and peer-reviews for another 13 journals. She has received several large competitive grants, most recently being awarded in excess of $400,00 in an industry led grant from the Australia Chiropractors Association to perform a longitudinal study on back pain in older Australians who present to a chiropractor for treatment of their low back pain. She has won many research prizes, including 1st prize at the World Federation of Chiropractic Biennial Conference in Washington DC (March, 2017). She is actively on the board for the Chiropractic Australia Research Foundation, and is the Research Chair for Sports Chiropractic Australia. She is one of only 13 CARL Fellows, a group which she is privileged to be a part of. She hopes to be a leading chiropractic researcher on spinal pain in the elderly.
View Dr. de Luca’s research at researchgate.net.
Here are the articles we discuss in this interview:
| 1. | Qualitative insights into the experience of pain in older Australian women with arthritis. |
| de Luca K, Parkinson L, Hunter S, Byles JE. | |
| Australas J Ageing. 2018 Sep;37(3):210-216. doi: 10.1111/ajag.12557. Epub 2018 Jun 26. | |
| PMID: 29947165 [PubMed – in process] | |
| Similar articles |
| 2. | The Relationship Between Spinal Pain and Comorbidity: A Cross-sectional Analysis of 579 Community-Dwelling, Older Australian Women. |
| de Luca KE, Parkinson L, Haldeman S, Byles JE, Blyth F. | |
| J Manipulative Physiol Ther. 2017 Sep;40(7):459-466. doi: 10.1016/j.jmpt.2017.06.004. Epub 2017 Oct 13. | |
| PMID: 29037787 [PubMed – indexed for MEDLINE] | |
| Similar articles |
| 3. | Three subgroups of pain profiles identified in 227 women with arthritis: a latent class analysis. |
| de Luca K, Parkinson L, Downie A, Blyth F, Byles J. | |
| Clin Rheumatol. 2017 Mar;36(3):625-634. doi: 10.1007/s10067-016-3343-5. Epub 2016 Jul 6. | |
| PMID: 27383742 [PubMed – indexed for MEDLINE] | |
| Similar articles |
 Geoffrey Bove, DC, PhD, and I discuss his research regarding inflammation within peripheral nerves, chiropractic principles, manual therapies, repetitive motion disorders and much more. Dr. Bove is a graduate of Hampshire College, Canadian Memorial Chiropractic College, and the University of North Carolina, Chapel Hill. He is currently a professor at the University of New England, in Biddeford Maine (USA). Dr. Bove’s research has focused on the effect of inflammation on small diameter axons within peripheral nerves, a topic directed by founding chiropractic principles. He also studies the effects of manual therapies on common painful conditions, such as repetitive motion disorders and postoperative visceral adhesions.
Geoffrey Bove, DC, PhD, and I discuss his research regarding inflammation within peripheral nerves, chiropractic principles, manual therapies, repetitive motion disorders and much more. Dr. Bove is a graduate of Hampshire College, Canadian Memorial Chiropractic College, and the University of North Carolina, Chapel Hill. He is currently a professor at the University of New England, in Biddeford Maine (USA). Dr. Bove’s research has focused on the effect of inflammation on small diameter axons within peripheral nerves, a topic directed by founding chiropractic principles. He also studies the effects of manual therapies on common painful conditions, such as repetitive motion disorders and postoperative visceral adhesions.
Visit Dr. Bove’s research gate profile.
Here are the links to Dr. Bove’s articles we discuss in this interview:
| 1. | Time course of ongoing activity during neuritis and following axonal transport disruption. |
| Satkeviciute I, Goodwin G, Bove GM, Dilley A. | |
| J Neurophysiol. 2018 May 1;119(5):1993-2000. doi: 10.1152/jn.00882.2017. Epub 2018 Feb 21. | |
| PMID: 29465329 [PubMed – in process] | |
| Similar articles |
| 2. | Group IV nociceptors develop axonal chemical sensitivity during neuritis and following treatment of the sciatic nerve with vinblastine. |
| Govea RM, Barbe MF, Bove GM. | |
| J Neurophysiol. 2017 Oct 1;118(4):2103-2109. doi: 10.1152/jn.00395.2017. Epub 2017 Jul 12. | |
| PMID: 28701542 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
| 3. | Attenuation of postoperative adhesions using a modeled manual therapy. |
| Bove GM, Chapelle SL, Hanlon KE, Diamond MP, Mokler DJ. | |
| PLoS One. 2017 Jun 2;12(6):e0178407. doi: 10.1371/journal.pone.0178407. eCollection 2017. | |
| PMID: 28574997 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
| 4. | A model for radiating leg pain of endometriosis. |
| Bove GM. | |
| J Bodyw Mov Ther. 2016 Oct;20(4):931-936. doi: 10.1016/j.jbmt.2016.04.013. Epub 2016 Apr 14. | |
| PMID: 27814877 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
| 5. | A Novel Method for Evaluating Postoperative Adhesions in Rats. |
| Bove GM, Chapelle SL, Boyle E, Mokler DJ, Hartvigsen J. | |
| J Invest Surg. 2017 Apr;30(2):88-94. doi: 10.1080/08941939.2016.1229367. Epub 2016 Oct 3. | |
| PMID: 27690703 [PubMed – indexed for MEDLINE] | |
| Similar articles |
| 6. | Manual therapy as an effective treatment for fibrosis in a rat model of upper extremity overuse injury. |
| Bove GM, Harris MY, Zhao H, Barbe MF. | |
| J Neurol Sci. 2016 Feb 15;361:168-80. doi: 10.1016/j.jns.2015.12.029. Epub 2015 Dec 24. | |
| PMID: 26810536 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
| 7. | Disruption of fast axonal transport in the rat induces behavioral changes consistent with neuropathic pain. |
| Dilley A, Richards N, Pulman KG, Bove GM. | |
| J Pain. 2013 Nov;14(11):1437-49. doi: 10.1016/j.jpain.2013.07.005. Epub 2013 Sep 12. | |
| PMID: 24035352 [PubMed – indexed for MEDLINE] | |
| Similar articles |
| 8. | Focal nerve inflammation induces neuronal signs consistent with symptoms of early complex regional pain syndromes. |
| Bove GM. | |
| Exp Neurol. 2009 Sep;219(1):223-7. doi: 10.1016/j.expneurol.2009.05. |
|
| PMID: 19477176 [PubMed – indexed for MEDLINE] | |
| Similar articles |
| 9. | Inflammation induces ectopic mechanical sensitivity in axons of nociceptors innervating deep tissues. |
| Bove GM, Ransil BJ, Lin HC, Leem JG. | |
| J Neurophysiol. 2003 Sep;90(3):1949-55. Epub 2003 Apr 30. | |
| PMID: 12724363 [PubMed – indexed for MEDLINE] Free Article | |
| Similar articles |
| 10. | Disruption of axoplasmic transport induces mechanical sensitivity in intact rat C-fibre nociceptor axons. |
| Dilley A, Bove GM. | |
| J Physiol. 2008 Jan 15;586(2):593-604. Epub 2007 Nov 15. | |
| PMID: 18006580 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
 Dr. Craig Moore discusses the role of chiropractors in the management of headaches. Some areas of discussion we touch upon include the societal impact and costs associated with headaches; prevalence of headaches in the community; prevalence of headache in chiropractic clinical settings; why do people turn to chiropractors; current level of evidence for chiropractic treatment of different headache types; what do the headache guidelines recommend for each headache; what should a chiropractor consider when examining a headache patient (history and examination).
Dr. Craig Moore discusses the role of chiropractors in the management of headaches. Some areas of discussion we touch upon include the societal impact and costs associated with headaches; prevalence of headaches in the community; prevalence of headache in chiropractic clinical settings; why do people turn to chiropractors; current level of evidence for chiropractic treatment of different headache types; what do the headache guidelines recommend for each headache; what should a chiropractor consider when examining a headache patient (history and examination).
Dr. Craig Moore is the director of a multi-disciplinary allied-health clinic in Crows Nest, Sydney. His clinic focus is toward the diagnosis and management of musculoskeletal disorders and in headache disorders in particular (migraine, tension-type headache, cervicogenic headache).
Dr. Moore has completed a Masters of Clinical Trials Research and is currently enrolled at the University of Technology Sydney, doing a PhD in Public Health – focused on the chiropractic management of headache disorders. As a founding member of the Australian Chiropractic Research Network (ACORN) he has a strong interest in supporting the development of chiropractic research through the utilization of this practice-based research network project. He has numerous publications in the scientific literature in such journals as Spine, BMC Neurology, JMPT, BMC Musculoskeletal Disorders and Headache to name a few. Dr. Moore is also a CARL Fellow!
See Dr. Moore’s research at researchgate.net.
Here are the articles we mentioned during the podcast:
| 1. | The treatment of migraine patients within chiropractic: analysis of a nationally representative survey of 1869 chiropractors. |
| Moore C, Adams J, Leaver A, Lauche R, Sibbritt D. | |
| BMC Complement Altern Med. 2017 Dec 4;17(1):519. doi: 10.1186/s12906-017-2026-3. | |
| PMID: 29202816 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
| 2. | A cross-sectional examination of the profile of chiropractors recruited to the Australian Chiropractic Research Network (ACORN): a sustainable resource for future chiropractic research. |
| Adams J, Peng W, Steel A, Lauche R, Moore C, Amorin-Woods L, Sibbritt D. | |
| BMJ Open. 2017 Sep 29;7(9):e015830. doi: 10.1136/bmjopen-2017-015830. | |
| PMID: 28965091 [PubMed – in process] Free PMC Article | |
| Similar articles |
| 3. | The Prevalence, Patterns, and Predictors of Chiropractic Use Among US Adults: Results From the 2012 National Health Interview Survey. |
| Adams J, Peng W, Cramer H, Sundberg T, Moore C, Amorin-Woods L, Sibbritt D, Lauche R. | |
| Spine (Phila Pa 1976). 2017 Dec 1;42(23):1810-1816. doi: 10.1097/BRS.0000000000002218. | |
| PMID: 28459779 [PubMed – in process] | |
| Similar articles |
| 4. | A critical review of manual therapy use for headache disorders: prevalence, profiles, motivations, communication and self-reported effectiveness. |
| Moore CS, Sibbritt DW, Adams J. | |
| BMC Neurol. 2017 Mar 24;17(1):61. doi: 10.1186/s12883-017-0835-0. Review. | |
| PMID: 28340566 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
| 5. | A workforce survey of Australian chiropractic: the profile and practice features of a nationally representative sample of 2,005 chiropractors. |
| Adams J, Lauche R, Peng W, Steel A, Moore C, Amorin-Woods LG, Sibbritt D. | |
| BMC Complement Altern Med. 2017 Jan 5;17(1):14. doi: 10.1186/s12906-016-1542-x. | |
| PMID: 28056964 [PubMed – indexed for MEDLINE] Free PMC Article | |
| Similar articles |
Partner
Donate
Recent Episodes
- 073 – Chiropractic Headache Guideline – Tension-Type and Cervicogenic with Dr. Robert Trager March 15, 2026
- 072- Neck Pain, Medicare, Costs, Adverse Events with Drs. Jim Whedon and Brian Anderson November 13, 2025
- 071- Dr. Cesar Hincapie – Chiropractic, Lumbar Disc Herniations, Nerve Root Injections September 30, 2025
- 070- Dr. Alice Cade – Chiropractic, Eye Tracking and Mild Traumatic Brain Injury June 26, 2025
- 069 – Dr. Walter Herzog – Biomechanics, Spinal Manipulation, Vertebral Artery and Gait March 13, 2025
- 068- Dr. Felipe Duarte – Neurobiology related to chronic musculoskeletal conditions and spinal manipulation November 21, 2024
- 067- Dr. Caroline Fagundes Discusses Vertebral Artery Strain, Posture and Falls October 15, 2024
- 066- Dr. Ronald Farabaugh – The Cost of Chiropractic vs Medical Management of Adults With Spine-Related Musculoskeletal Pain March 19, 2024
Security – SSL Certificate
Partner
 Chiropractic Science is a Miami University Digital Health Literacy Partner. Health literacy is the ability to read, write, and talk about health habits in a variety of life situations and environments. Our interprofessional partnership promotes the use and dissemination of electronic materials for evidence-based EHealth.
Chiropractic Science is a Miami University Digital Health Literacy Partner. Health literacy is the ability to read, write, and talk about health habits in a variety of life situations and environments. Our interprofessional partnership promotes the use and dissemination of electronic materials for evidence-based EHealth.


