 In this update, I will summarize key points from recent scientific literature regarding the practice of chiropractic, patient profiles, utilization rates, chiropractic assessment and care methods. Much of the information comes from the excellent work of Beliveau et al (2017) who did a scoping review and used 337 articles from across the globe. I have provided references to other key papers also.
In this update, I will summarize key points from recent scientific literature regarding the practice of chiropractic, patient profiles, utilization rates, chiropractic assessment and care methods. Much of the information comes from the excellent work of Beliveau et al (2017) who did a scoping review and used 337 articles from across the globe. I have provided references to other key papers also.
Chiropractors practice in over 100 countries. There are 90 existing national chiropractic associations across the world. Chiropractic has become one of the most commonly used health professions in the United States and Europe. A substantial proportion of US adults utilize chiropractic services and report associated positive outcomes for overall well-being and/or specific health problems for which concurrent conventional care was common (1). Chiropractors provide a significant amount of care for patients with many health conditions including low back and neck pain. The profession is a major participant in the health care expenditures of the United States and Denmark. As an example, here in the United States in 2015, chiropractors provided 18.6 million clinical services under Medicare and overall spending for chiropractic services was estimated at USD $12.5 billion (Beliveau et al, 2017).
According to the American Chiropractic Association (2), there are 77,000 chiropractors in the United States with roughly another 3,000 chiropractors that work in academic and management roles. There are approximately 10,000 chiropractic students in 18 nationally accredited, chiropractic doctoral programs across the United States with 2,500 chiropractors entering the work environment each year. Estimates indicate that chiropractors treat more than 35 million Americans (adults and children) annually. Chiropractors are designated as physician-level providers in the vast majority of states and the federal Medicare program. The essential services provided by chiropractors are also available in federal health delivery systems, including those administered by Medicaid, the U.S. Departments of Veterans Affairs (VA) and Defense, Federal Employees Health Benefits Program, Federal Workers’ Compensation, and all state workers’ compensation programs. Chiropractic is currently offered at 75 VA facilities and 66 military hospitals/clinics.
National and international guidelines include chiropractic (spinal manipulation) for low back pain (LBP) and neck pain. A short summary (3-4) of recent guidelines include:
- For acute and chronic LBP, a review of clinical practice guidelines (CPGs) on the noninvasive management of LBP and 3 national CPGs published since 2016 in the United States (Agency for Healthcare Research and Quality [AHRQ] comparative effectiveness review [CER]), the UK (National Institute for Care Excellence [NICE]), and Denmark (Denmark National Guideline) recommend considering manual therapy, including SMT, mobilization, or soft tissue techniques such as massage
- An additional CPG, by the American College of Physicians (ACP), recommends clinicians select nonpharmacologic treatment for acute and chronic LBP (superficial heat, massage, acupuncture, and SMT) before pharmacologic treatment options
Chiropractic utilization rates
- Across the world, 52 studies (Beliveau et al, 2017) have found the median 12-month use of chiropractic services was 9.1% and lifetime utilization was 22.2%
- In Canada and the United States there has been an increased 12 month utilization rate from 10% to 11.7% and from 7.2% to 10.7% respectively from the 1980’s until 2015
Who delivers spinal manipulation?
- Among the 8.5% of US adults who reported receiving manipulation, 97.6% saw chiropractors according to the 2012 National Health Interview Survey (5)
Reasons for seeing a chiropractor
- For the general population, the most common reasons for seeking care from a chiropractor included: low back pain (49.7%), neck pain (22.5%), extremity problem (10%), wellness/maintenance (7.5%), hip pain (7%), headache (5.5%)
- For the pediatric population, the most common reasons for seeking care from a chiropractor included: musculoskeletal conditions (44%), excessive crying (19.8%), neurologic conditions (17.9%), gastrointestinal conditions (17.5%), ear/nose/throat conditions (8.3%) and infection (7%) (Beliveau et al, 2017)
Profile of chiropractic patients
- People who sought chiropractic care were more likely to be female with a median age of 43.4 years
- 3% of the chiropractic patient population were employed, and a smaller proportion were either retired, unemployed, or students
- People with disabilities constituted only 1.4% of chiropractic patients (Beliveau et al, 2017)
Types of chiropractic assessments used in practice
- The most common assessment methods included: static palpation (89.3%), motion palpation (86.5%), spinal examination (79.5%), orthopedic examination (71.8%), neurological examination (64.6%) (Beliveau et al, 2017)
Types of chiropractic treatment provided
- Across the globe, spinal manipulation (79.3%), soft-tissue therapy (35.1%), formal patient education (31.3%), nutritional supplements (30.9%), exercise instruction/prescription (26%)
- Interestingly the NBCE (National Board of Chiropractic Examiners) found that in the US: 98.8% of chiropractors provide ergonomic/postural advice, 98.5% of chiropractors provide physical fitness/exercise promotion and 97% of chiropractors provide nutritional/dietary recommendations (Beliveau et al, 2017)
References:
Main Source: Beliveau PJH, Wong JJ, Sutton DA et al. The chiropractic profession: a scoping review of utilization rates, reasons for seeking care, patient profiles, and care provided. Chiropr Man Therap. 2017 Nov 22;25:35.
1. Adams J, Peng W, Cramer H, Sundberg T, Moore C, Amorin-Woods L, Sibbritt D, Lauche R. The Prevalence, Patterns, and Predictors of Chiropractic Use Among US Adults: Results From the 2012 National Health Interview Survey. Spine (Phila Pa 1976). 2017 Dec 1;42(23):1810-1816.
2. https://www.acatoday.org/Patients/Why-Choose-Chiropractic/Key-Facts
3. Wong JJ, Côté P, Sutton DA, et al. Clinical practice guidelines for the noninvasive management of low back pain: A systematic review by the Ontario Protocol for Traffic Injury Management (OPTIMa) Collaboration. Eur J Pain 2016;21(2):201-16.
4. Bussières AE, Gauthier CA, Fournier G, Descarreaux M. Spinal manipulative therapy for low back pain-time for an update. Can Fam Physician. 2017 Sep;63(9):669-672.
5. Forte ML, Maiers M. Functional Limitations in Adults Who Utilize Chiropractic or Osteopathic Manipulation in the United States: Analysis of the 2012 National Health Interview Survey. J Manipulative Physiol Ther. 2017 Nov -Dec;40(9):668-675.



 Upcoming interview with Dr. Katie de Luca. Katie de Luca is a post-doctoral research fellow in the Department of Chiropractic at Macquarie University. She is a chiropractor in clinical practice, however her research focuses on the epidemiology and management of musculoskeletal conditions, with expertise in the elderly. In 2016 she was awarded her PhD from the University of Newcastle, School of Medicine and Public Health. Her thesis explored the experience of pain in women with arthritis, and resulted in substantial contributions to fields of rheumatology, pain and ageing research. She has 25 peer-reviewed journal publications and more than 50 conference presentations, which includes several invited keynote presentations on back pain in the elderly. These have been at regional, national and international conferences in gerontology, pain, public health and chiropractic forums. She is on the editorial boards of Chiropractic and Manual Therapies and JMPT, and peer-reviews for another 13 journals. Please comment below if you have any questions for us during the interview. I might choose some of them for our conversation.
Upcoming interview with Dr. Katie de Luca. Katie de Luca is a post-doctoral research fellow in the Department of Chiropractic at Macquarie University. She is a chiropractor in clinical practice, however her research focuses on the epidemiology and management of musculoskeletal conditions, with expertise in the elderly. In 2016 she was awarded her PhD from the University of Newcastle, School of Medicine and Public Health. Her thesis explored the experience of pain in women with arthritis, and resulted in substantial contributions to fields of rheumatology, pain and ageing research. She has 25 peer-reviewed journal publications and more than 50 conference presentations, which includes several invited keynote presentations on back pain in the elderly. These have been at regional, national and international conferences in gerontology, pain, public health and chiropractic forums. She is on the editorial boards of Chiropractic and Manual Therapies and JMPT, and peer-reviews for another 13 journals. Please comment below if you have any questions for us during the interview. I might choose some of them for our conversation. In this upcoming interview, Alice Kongsted, DC, PhD will discuss how the bio-medical/structural approach to back pain has failed and we need to implement a behavioural approach to back pain much more in practice. She will discuss the recommendation of active, non-pharmacological treatments that support self-management. Dr. Kongsted was part of the Lancet Low Back Pain Series Working Group that published three papers in March 2018 to call for worldwide recognition of the disability associated with back pain and the need for prioritizing this globally growing problem. Please comment below if you have any questions for us during the interview. I might choose some of them for our conversation.
In this upcoming interview, Alice Kongsted, DC, PhD will discuss how the bio-medical/structural approach to back pain has failed and we need to implement a behavioural approach to back pain much more in practice. She will discuss the recommendation of active, non-pharmacological treatments that support self-management. Dr. Kongsted was part of the Lancet Low Back Pain Series Working Group that published three papers in March 2018 to call for worldwide recognition of the disability associated with back pain and the need for prioritizing this globally growing problem. Please comment below if you have any questions for us during the interview. I might choose some of them for our conversation. There is a growing trend of chiropractic use in adults.
There is a growing trend of chiropractic use in adults.  In this update, I will summarize key points from recent scientific literature regarding the practice of chiropractic, patient profiles, utilization rates, chiropractic assessment and care methods. Much of the information comes from the excellent work of
In this update, I will summarize key points from recent scientific literature regarding the practice of chiropractic, patient profiles, utilization rates, chiropractic assessment and care methods. Much of the information comes from the excellent work of  Today, we celebrate the birthday of the chiropractic profession, Sept. 18. Chiropractic’s first adjustment is recognized each year as Chiropractic Founder’s Day. On this day in 1895 (122 years ago), Dr. Daniel David Palmer gave the first chiropractic adjustment. Chiropractic is a health profession concerned with the assessment, care and prevention of disorders of the musculoskeletal system and the effects of these disorders on the nervous system and general health.
Today, we celebrate the birthday of the chiropractic profession, Sept. 18. Chiropractic’s first adjustment is recognized each year as Chiropractic Founder’s Day. On this day in 1895 (122 years ago), Dr. Daniel David Palmer gave the first chiropractic adjustment. Chiropractic is a health profession concerned with the assessment, care and prevention of disorders of the musculoskeletal system and the effects of these disorders on the nervous system and general health.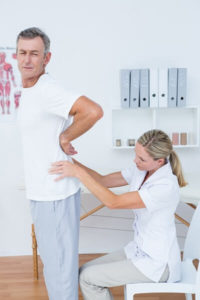 There was a low recurrence rate (using a stringent definition of recurrence) in a large population of patients with low back pain (LBP) up to 1 year after chiropractic care. However, the vast majority of patients were not pain free after 1 year. This is the conclusion of a recent observational study published in the
There was a low recurrence rate (using a stringent definition of recurrence) in a large population of patients with low back pain (LBP) up to 1 year after chiropractic care. However, the vast majority of patients were not pain free after 1 year. This is the conclusion of a recent observational study published in the 
