 American chiropractors are very similar to chiropractors in other countries, as well as other health professionals in terms of their favorable attitudes towards evidence based practice (EBP) (1-2). The purpose of EBP is to promote effective chiropractic practice and enhance public health. Evidence based practice incorporates the best research evidence with individual clinical expertise and patient choice/values (3). There are however several limitations and barriers to implementing EBP that chiropractors express such as lack of research relevance, lack of time and insufficient skills for locating and appraising research (1). It is important to note that these same obstacles are also encountered by other professions including medicine and nursing.
American chiropractors are very similar to chiropractors in other countries, as well as other health professionals in terms of their favorable attitudes towards evidence based practice (EBP) (1-2). The purpose of EBP is to promote effective chiropractic practice and enhance public health. Evidence based practice incorporates the best research evidence with individual clinical expertise and patient choice/values (3). There are however several limitations and barriers to implementing EBP that chiropractors express such as lack of research relevance, lack of time and insufficient skills for locating and appraising research (1). It is important to note that these same obstacles are also encountered by other professions including medicine and nursing.
In a recent survey, very few DCs indicated that computer, internet, or database access were barriers to their uptake of EBP (1). Since chiropractors are interested in implementing EBP, these findings underscore the importance of providing clinicians with training in EBP skills, particularly through online resources. It is likely that comprehensive and multi-faceted approaches that take into account all the relevant levels affecting EBP will likely be needed to integrate research into practice (1).
As a practitioner as well as a researcher, I realize the importance and barriers of translating research into practice. I have also begun to realize how I can give back to the profession. Some of you may recognize my On Target research summaries. Others may be familiar with my chiropractic science podcast. While there may be many ways to tackle the evidence-practice gap, one convenient educational method is a podcast. This is one of the ways that I have been utilizing to help get chiropractic research out to the masses. For those not familiar, a podcast describes audio and/or video files that can be downloaded and played on a personal computer or mobile device.
Podcast is the term commonly used to refer to a series of digital media files that are released periodically and can be subscribed to using an RSS (Really Simple Syndication) feed. This means of digital delivery is what makes podcasting different from other means of accessing media files over the internet. Of course one can still download the audio and/or video files that makeup a podcast. The automatically downloaded files can be stored locally on a computer or other device (such as your mobile phone) ready for offline use, providing simple and convenient access to regular releases.
Podcasting has been used successfully in teaching and learning in many different student groups (4-5). In theory podcasts provide educational content in a format that is convenient and available 24 hours a day and can be accessed whenever and wherever the learner chooses (4-5). Learners have the ability to replay a podcast as many times as they wish in order to improve understanding. In addition, podcasting offers the ability to embed additional content from researchers or clinicians to help make links between theoretical concepts and practice.
While many chiropractic podcasts exist, chiropractic science (CS) is the only podcast that exclusively interviews chiropractic researchers about the science of chiropractic. CS publicizes and disseminates chiropractic research. Hear about chiropractic research from the authors in plain English, not through the media, nor a middleman. Think about recent media coverage concerning the evidence of chiropractic in magazines or online. While reports of chiropractic studies in the media may be very good (or very poor), some things get lost in translation. By interviewing the chiropractic experts that are actually doing the research, you’ll get the information direct – the way the author intended it.
Making scientific findings available to the public is an important part of the research process. Publicizing these interviews passes on the benefits of chiropractic research to other researchers, chiropractors in practice as well as practitioners from other disciplines and the wider community. In addition to publicizing the interviews, other goals of the podcast are to encourage collaboration of researchers to promote future high quality chiropractic research as well as to motivate and assist practitioners and students alike to pursue research careers in chiropractic science!
Why Chiropractic Science?
- There is a lot of excellent chiropractic research published by top scientists in the field that deserve our attention
- Incorporating the latest evidence into your practice of chiropractic is good for everyone
- Reduce the evidence – practice gap and promote knowledge translation from the chiropractic research laboratory to the clinic
- Engage clinicians in evidence based practice in a fun, easy to access manner
- Learn from the experts and gain confidence in your knowledge and communications with others about chiropractic
- A chiropractic resource for students, doctors and patients
Feedback about Chiropractic Science
- “It has been such an inspiration to listen to all the greats in the world of chiropractic research”
- “It has certainly made an impact on my practice and gives me a tremendous amount of certainty in what we do as chiropractors”
- “I find the information profoundly motivating”
- “It is difficult to read and interpret journal articles for a seasoned chiropractor. This saves time and hearing it explained from your colleagues themselves in language that I can communicate with my patients is invaluable”
- “I am humbled by the sacrifice, hard work and accomplishments of all the researchers you have interviewed”
- “Being in practice for many years, I am weary of ideologically biased forums when 21st Century chiropractic can have and bring it all; evidence and practice based science WITH a strong philosophical foundation. Highest accolades to Dr. Dean Smith for his untiring success at bringing the bar, raising colleagues and conversations together to articulate just how pertinent chiropractic is in contemporary health care”
In short, CS is starting to achieve what it set out to do, but this just the beginning. I am humbled by the feedback I have received from chiropractors about the podcast and am looking forward to interviewing as many chiropractic researchers as possible. If you haven’t listened to the podcast, check them out. If you like what you hear, please leave a great review on iTunes. This will help position CS as a leading health podcast – enlightening the masses about the evidence of chiropractic. Listen to the podcast on iTunes or download the files directly to your device from chiropracticscience.com. Enjoy and share with everyone.
References:
- Schneider MJ, Evans R, Haas M, Leach M, Hawk C, Long C, Cramer GD, Walters O, Vihstadt C, Terhorst L. US chiropractors’ attitudes, skills and use of evidence-based practice: A cross-sectional national survey. Chiropr Man Therap. 2015 May 4;23:16.
- Alcantara J, Leach MJ. Chiropractic Attitudes and Utilization of Evidence-Based Practice: The Use of the EBASE Questionnaire. Explore (NY). 2015 Sep-Oct;11(5):367-76.
- Lefebvre R, Peterson D, Haas M. Evidence-Based Practice and Chiropractic Care. J Evid Based Complementary Altern Med. 2012 Dec 28;18(1):75-79.
- Burke S, Cody W. Podcasting in undergraduate nursing programs. Nurse Educ. 2014 Sep-Oct;39(5):256-9.
- Strickland K, Gray C, Hill G. The use of podcasts to enhance research-teaching linkages in undergraduate nursing students. Nurse Educ Pract. 2012 Jul;12(4):210-4.
Dr. Dean Smith is founder of chiropractic science – dedicated to publicizing and disseminating chiropractic research through podcast interviews with the experts that are doing the research. Listen to free chiropracticscience.com interviews on iTunes. Dr. Smith is also a clinical professor at Miami University in Oxford, Ohio. He has a practice of chiropractic in Eaton, Ohio.

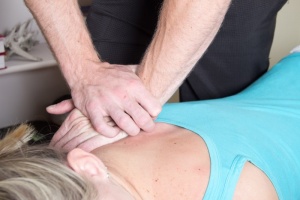 Spinal manipulation (SM) can improve function and reduce spinal disability. SM also provides pain relief for many disorders such as back pain and neck pain. Pain induces changes in both the central and peripheral nervous systems. The mechanisms by which SM alters musculoskeletal pain are still not completely known. Current evidence however suggests that SM is associated with neurophysiological responses including rapid hypoalgesia with simultaneous sympathetic and motor system excitation. Animal studies have shown that analgesia provided by joint mobilization involves serotonin and noradrenaline receptors in the spinal cord.
Spinal manipulation (SM) can improve function and reduce spinal disability. SM also provides pain relief for many disorders such as back pain and neck pain. Pain induces changes in both the central and peripheral nervous systems. The mechanisms by which SM alters musculoskeletal pain are still not completely known. Current evidence however suggests that SM is associated with neurophysiological responses including rapid hypoalgesia with simultaneous sympathetic and motor system excitation. Animal studies have shown that analgesia provided by joint mobilization involves serotonin and noradrenaline receptors in the spinal cord. Chiropractors, how do you take all of the current chiropractic research and develop an effective evidence based practice strategy? I will be joining Dr. Stu Hoffman and ChiroSecure next Tuesday, June 21st for The Importance of an Evidence Based Practice.
Chiropractors, how do you take all of the current chiropractic research and develop an effective evidence based practice strategy? I will be joining Dr. Stu Hoffman and ChiroSecure next Tuesday, June 21st for The Importance of an Evidence Based Practice.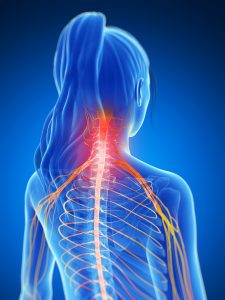 The application of spinal manipulative therapy (SMT) is a cost-effective and widely recognized manual intervention used by a variety of health care professionals in the management of musculoskeletal pain. A growing body of scientific evidence supports the use of SMT for the treatment of a broad range of musculoskeletal disorders citing short-term antinociceptive (pain-relieving) effects and restoration of normal joint mechanics.
The application of spinal manipulative therapy (SMT) is a cost-effective and widely recognized manual intervention used by a variety of health care professionals in the management of musculoskeletal pain. A growing body of scientific evidence supports the use of SMT for the treatment of a broad range of musculoskeletal disorders citing short-term antinociceptive (pain-relieving) effects and restoration of normal joint mechanics. Musculoskeletal pain in pregnant women is common and is frequently viewed as short-lived and temporary. Most women report either low back pain (LBP) or pelvic pain (PP) during pregnancy and up to 40% of patients report pain during the 18 months after delivery. Pelvic pain in pregnant women is a health care challenge in which moderate and severe pain develops rather early and has important implications for society. These pain syndromes increase sick leave and impair general level of function during pregnancy.
Musculoskeletal pain in pregnant women is common and is frequently viewed as short-lived and temporary. Most women report either low back pain (LBP) or pelvic pain (PP) during pregnancy and up to 40% of patients report pain during the 18 months after delivery. Pelvic pain in pregnant women is a health care challenge in which moderate and severe pain develops rather early and has important implications for society. These pain syndromes increase sick leave and impair general level of function during pregnancy. Research on chiropractic spinal manipulation (CSM) has been conducted extensively worldwide, and its efficacy on musculoskeletal symptoms has been well documented. Previous studies have documented potential relationships between spinal dysfunction and the autonomic nervous system and that chiropractic treatment affects the autonomic nervous system.
Research on chiropractic spinal manipulation (CSM) has been conducted extensively worldwide, and its efficacy on musculoskeletal symptoms has been well documented. Previous studies have documented potential relationships between spinal dysfunction and the autonomic nervous system and that chiropractic treatment affects the autonomic nervous system.  In
In 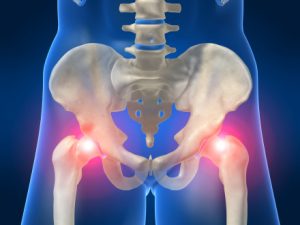 Chiropractic care holds potential value for the treatment of a variety of limb conditions. For patients with osteoarthritis (OA) of the hip, a combined intervention of manual therapy provided by a chiropractor and patient education was more effective than a minimal control intervention.
Chiropractic care holds potential value for the treatment of a variety of limb conditions. For patients with osteoarthritis (OA) of the hip, a combined intervention of manual therapy provided by a chiropractor and patient education was more effective than a minimal control intervention. Over the last decade, research has demonstrated that spinal manipulation can change various aspects of nervous system function, including muscle reflexes, cognitive processing, reaction time, and the speed at which the brain processes information. One research group from New Zealand (Haavik et al) has hypothesized that the joint dysfunction part of the chiropractic clinical construct, the vertebral subluxation, results in altered afferent input to the central nervous system (CNS) that modifies the way in which the CNS processes and integrates all subsequent sensory input. This processing (i.e., sensorimotor integration) is a central nervous system (CNS) function that appears most vulnerable to altered inputs.
Over the last decade, research has demonstrated that spinal manipulation can change various aspects of nervous system function, including muscle reflexes, cognitive processing, reaction time, and the speed at which the brain processes information. One research group from New Zealand (Haavik et al) has hypothesized that the joint dysfunction part of the chiropractic clinical construct, the vertebral subluxation, results in altered afferent input to the central nervous system (CNS) that modifies the way in which the CNS processes and integrates all subsequent sensory input. This processing (i.e., sensorimotor integration) is a central nervous system (CNS) function that appears most vulnerable to altered inputs.
