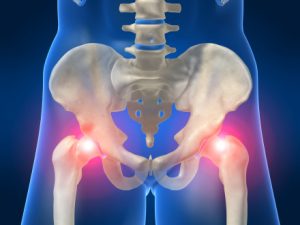
Hip Osteoarthritis – Improvements in Pain and Disability with Care Provided by a Chiropractor
 Chiropractic care holds potential value for the treatment of a variety of limb conditions. For patients with osteoarthritis (OA) of the hip, a combined intervention of manual therapy provided by a chiropractor and patient education was more effective than a minimal control intervention.
Chiropractic care holds potential value for the treatment of a variety of limb conditions. For patients with osteoarthritis (OA) of the hip, a combined intervention of manual therapy provided by a chiropractor and patient education was more effective than a minimal control intervention.
A recent article by Poulsen et al (2013) contributes to our understanding of the literature regarding chiropractic and lower extremity conditions – particularly hip osteoarthritis. Hip osteoarthritis (OA) is a common joint disease and when symptomatic can have significant impact on regular daily activities. Recently, hip OA has been linked to higher mortality rates. In end stage hip OA, joint replacement surgery is an appropriate and cost-effective treatment but a long-term cohort study has documented that only 20% of patients with radiographic hip OA have had surgery 11-28 years after the initial diagnosis. Therefore, non-surgical interventions with documented effectiveness become essential for patients who do not need, or choose not to have surgery.
Although guidelines recommend patient education (PE) programs as a core intervention, systematic reviews are contradictory in conclusions regarding their effectiveness on pain and function in hip OA. Manual therapy (MT) has been proposed as an adjunct intervention to exercise for patients with hip OA but evidence is based on a single randomized clinical trial (RCT). The authors of the current study realized this gap in the literature and decided to investigate the effectiveness of a patient education (PE) program with or without the added effect of manual therapy (MT) compared to a minimal control intervention (MCI).
The design of this study was a single-center proof-of-principle three-arm parallel group RCT. Inclusion criteria were: Unilateral hip pain >3 months’ duration, age 40-80 years, radiographic hip OA defined as minimal joint space width (JSW) measurement <2.00 mm or a side difference in minimal JSW >10%, and, ability to speak and read Danish. The study took place at the Department of Orthopaedic Surgery and Traumatology, Odense University Hospital, Denmark.
During the first 2 months of recruitment, 3 exclusion criteria were added to the original criteria: patients who had had MT within the previous twelve months; patients who rated their pain severity as 1 or 2 on the numerical rating scale (NRS); patients with polyarthritis.
The 3 groups in the study were: 1) MCI; 2) PE; 3) PE + MT.
For the MCI group, a nurse provided written advice on a home stretching program derived from the PE program together with 5-10-min instruction.
The PE group, originally termed ‘Hip School’ was taught by a physiotherapist with 11 years experience. The PE program included two individual sessions and three group sessions.
In the combined PE and MT group, manual therapy was administered by a chiropractor with 20 years of clinical experience. MT was scheduled twice a week for the 6-week intervention period and treatment was individualized to each patient depending on examination findings. MT consisted of: trigger point release therapy (TPPR), muscular stretching by muscle energy technique (MET) and joint manipulation.
The primary outcome was pain severity rated on an 11-box NRS, measured after 6 weeks of intervention. Patients were asked to rate the worst pain experienced during the previous week. Secondary outcome measures were the Hip Disability and Osteoarthritis Outcome Score (HOOS) ranging from 0-100, worst to best; patients’ perceived global effect of interventions, percentage in each group having classified themselves as improved; passive hip range of motion (ROM); use of pain medication at 12 months and hip replacement surgery within the 12 month follow-up period.
Results:
- A total of 111 patients were included in the analyses at the primary end point at 6 weeks
- In the combined group (PE + MT), a clinically relevant reduction in pain severity compared to the MCI of 1.90 points was achieved
- Effect size (Cohen’s d) for the PE + MT minus the MCI was 0.92 (large effect)
- The number of patients in each group experiencing pain reduction of at least 25% from baseline to 6 weeks was PE = 8, PE +MT = 21 and MCI = 7
- Number needed to treat for PE + MT was 3
- No difference was found between the PE and MCI groups
- At 12 months, not including patients receiving hip surgery the statistically significant difference favoring PE + MT was maintained
- All HOOS (pain, symptoms, ADLs, Sport/Rec, QOL) subscales demonstrated clinically relevant and statistically significant superiority, p < 0.05 for the PE + MT group when compared to the MCI group
- Mean differences between PE and MCI were small (range 4 to 1) and not statistically significant, p > 0.05
- Effect sizes for HOOS subscales for PE + MT minus MCI ranged between 0.75 and 1.08
- No changes in hip ROM noted between groups
Key Findings:
- For primary care patients with OA of the hip, a combined intervention of manual therapy provided by a chiropractor and patient education was more effective than a minimal control intervention
- Note that patient education alone was not superior to the minimal control intervention
So, what does this study tell us? This trial demonstrated clinical and statistically significant improvements in pain, symptoms and disability for a combined intervention consisting of manual therapy provided by a chiropractor and patient education when compared to a minimal control intervention including home stretching.
Reference: Poulsen E, Hartvigsen J, Christensen HW, Roos EM, Vach W, Overgaard S. Patient education with or without manual therapy compared to a control group in patients with osteoarthritis of the hip. A proof-of-principle three-arm parallel group randomized clinical trial. Osteoarthritis Cartilage. 2013 Oct;21(10):1494-503.